The United States is getting hit quite hard right now with the flu and flu-like viruses. It seems like a hopeless battle. What can you do to protect yourself? Are natural remedies bunk or beneficial? Here are 15 top natural tips, herbs, vitamins, and antiviral remedies you can take, to help build up your immune system and increase your ability to fight off the flu naturally.
The United States is getting hit quite hard right now with the flu and flu-like viruses. It seems like a hopeless battle. What can you do to protect yourself? Are natural remedies bunk or beneficial? Here are 15 top natural tips, herbs, vitamins, and antiviral remedies you can take, to help build up your immune system and increase your ability to fight off the flu naturally.
Continue reading
Tag Archives: vitamins
Understanding Epilepsy – Are Natural Treatments Effective?
What is epilepsy and how is it treated? Are there alternative or natural approaches to treating epilepsy? When it comes to the subject of epilepsy, many people find it difficult to fully understand the disorder and all of its characteristics. Even though signs of epilepsy in people were present centuries ago, epilepsy is a relatively new discovery in the world of health. Before the advancement of medical technology, those with epilepsy might have been look upon by others with confusion.
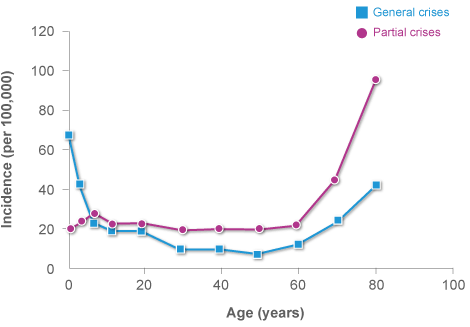
The Center of Disease Control & Prevention states that “2.3 million adults and 467,711 children (0-17 years of age) in the United States have epilepsy”. The incidence of the diagnosis of epilepsy has increased in the last few decades. There is a higher incidence of seizures among infants and elderly citizens over the age of 70.
What is Epilepsy? 
Epilepsy is a term used to express an array of brain disorders caused by seizures. Depending on the type of epilepsy, the disorder may be short-term or long-term. Epilepsy is characterized by a tendency for recurrent seizures. A seizure occurs when nerve cells in the brain signal abnormally causing temporary disruption in brain function. Neurons are overly stimulated which can lead to involuntary muscle spasms or convulsions, changes in behavior and/or changes in awareness or sensation. There are three main types of seizures: generalized seizures, partial or focal seizures and absence or petit mal seizures. Generalized seizures involve all parts of the brain. The Epilepsy Foundation provides the sub-types of generalized seizures in the following:
- Grand Mal Seizures- unconsciousness and convulsions
- Myoclonic Seizures- isolated jerking movements
- Clonic Seizures- repetitive jerking movements
- Tonic Seizures- muscle stiffness
- Atonic Seizures- loss of muscle tone
Symptoms Specific to Types of Seizures

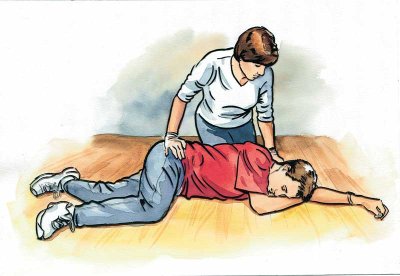
Generalized or tonic clonic seizures affect the entire brain. The person falls to the floor and shakes or twitches uncontrollably, and is unable to speak.
Generalized or Tonic-Clonic Seizures – With a generalized or tonic-clonic seizure, the person experiences muscle stiffness, loss of consciousness and/or flailing arms and legs. They may lose control of bowel or bladder, may have trouble breathing and turn blue or be foaming at the mouth.
The generalized seizure may last seconds or minutes. After the seizure, the person may feel very confused and it may take up to an hour for him/her to fully regain awareness of the situation.
Partial or Focal Seizures – During partial or focal seizures, part of the brain is affected. The part of the brain that is affected will determine which kind of symptoms arise. For example, if the occipital lobe is affected, the person may experience temporary blurry vision or is extremely sensitive to light. Within this category of seizures, there are also simple and complex partial seizures. Refer to diagrams A and B below.
A. Simple Partial Seizures
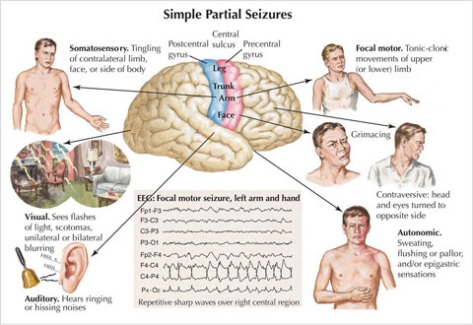
Simple partial seizure symptoms include arm twitching, tingling of face or one side of the body, seeing flashes of light, hearing ringing or hissing, sweating or flushing, facial grimacing or turning of head to one side.
B. Complex Partial Seizures
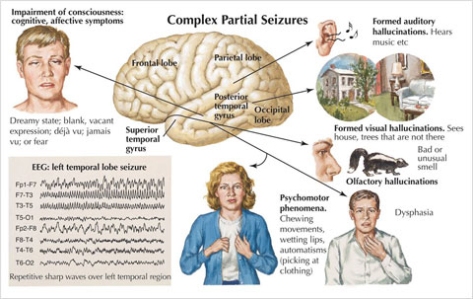
Complex partial seizure symptoms include chewing movements, wetting lips, and picking at clothing, dysphasia or trouble speaking, and auditory, visual or olfactory hallucinations.
 Absence seizures can occur many times in a day. People who have these seizures may exhibit moments of confusion, staring blanking and excessive blinking. Often absence or petit mal seizures go undetected because episodes can be brief but happen multiple times during the day or multiple times every hour. For more detailed information on each of the seizure types and symptoms, the Epilepsy Foundation is a very good resource.
Absence seizures can occur many times in a day. People who have these seizures may exhibit moments of confusion, staring blanking and excessive blinking. Often absence or petit mal seizures go undetected because episodes can be brief but happen multiple times during the day or multiple times every hour. For more detailed information on each of the seizure types and symptoms, the Epilepsy Foundation is a very good resource.
Types of Epilepsy
The type(s) of seizure(s) a person has dictates which type of epilepsy is present. Epilepsy is characterized by the types of seizures a person exhibits. The major types of epilepsy include but are not limited to the following:
- Idiopathic Generalized Epilepsy
- Childhood Absence Epilepsy
- Juvenile Myoclonic Epilepsy
- Photosensitive Epilepsy
- Benign Rolandic Epilepsy
Idiopathic Generalized Epilepsy
Since there are so many different types of epilepsy, we will focus on idiopathic generalized epilepsy (IGE) or primary generalized epilepsy. According to an article written by Selim Benbadis & Leanne Heriaud from Tampa General Hospital, entitled “Idiopathic Generalized Epilepsy,” patients with IGE experience the following type of seizures:
- Patients with IGE have one or more of 3 types of (primary generalized) seizures: myoclonic, absence and generalized tonic-clonic seizures.
- One type may be the only or main type in a given patient.
- Generalized tonic-clonic seizures are convulsions of the whole body lasting 1-2 minutes, and are the most common and most dramatic type of seizures.
- Absence seizures are brief staring spells with arrest of activity, often with eye fluttering, which last just a few seconds.
- Myoclonic seizures are very brief isolated body jerks that tend to occur in the morning.
Cause(s) of Idiopathic Generalized Epilepsy
Idiopathic generalized epilepsy is presumed to have a genetic cause however in many cases of epilepsy, a family history of the disorder may not be present. Patients with IGE who have a family history of the disorder may find it difficult to determine which family member will be born with IGE. The symptoms or seizures associated with IGE often start during childhood or adolescence. 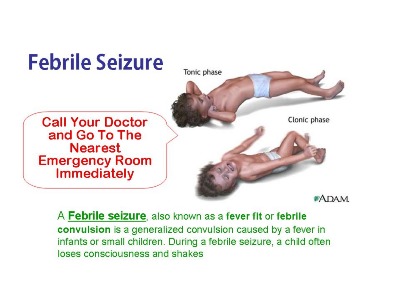 Seizures that occur during childhood and associated with high fevers are termed “febrile seizures,” and are not uncommon. Children and adults can have seizures and not be diagnosed with epilepsy. The diagnosis of epilepsy is not made after only one incidence of seizure, but instead it is made after recurrent episodes of seizures. The Center of Disease Control & Prevention offers some possible theories of events that may lead to epilepsy:
Seizures that occur during childhood and associated with high fevers are termed “febrile seizures,” and are not uncommon. Children and adults can have seizures and not be diagnosed with epilepsy. The diagnosis of epilepsy is not made after only one incidence of seizure, but instead it is made after recurrent episodes of seizures. The Center of Disease Control & Prevention offers some possible theories of events that may lead to epilepsy:
- Oxygen deprivation during childhood
- Brain infections such as meningitis, encephalitis, or brain abscessTraumatic brain injury or head injury
- Stroke resulting from a block or rupture of a vessel in the brain
- Other neurologic brain diseases such as Alzheimer Disease
- Brain Tumors
- Certain Genetic Disorders
Diagnosis of Idiopathic Generalized Epilepsy
For physicians, it’s challenging to exactly pinpoint the type of epilepsy a patient may have. Patients with IGE have normal intelligence and score in the normal range on neurological exams. One method to most accurately diagnose a patient with IGE is to perform electroencephalogram (EGG) tests.
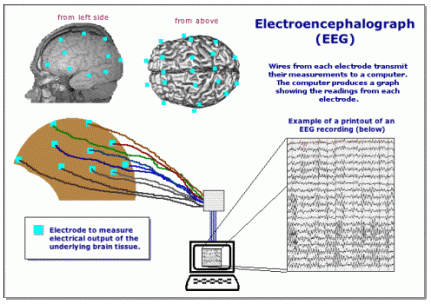 Flat metal discs are attached to the patient’s scalp to tract electrical activity in the brain. When the patient is having a seizure, the device documents the spikes. Other tests to assist physicians in diagnosing epilepsy include: Magnetic Resonance Testing (MRI), Positron Emissions Tomography (PET) Scan and Magnetic Resonance Spectroscopy (MRS). A good resource for more information about diagnostic tests for epilepsy is the John Hopkins Hospital School of Medicine, Neurology and Neurosurgery,“Diagnosing Seizures and Epilepsy.”
Flat metal discs are attached to the patient’s scalp to tract electrical activity in the brain. When the patient is having a seizure, the device documents the spikes. Other tests to assist physicians in diagnosing epilepsy include: Magnetic Resonance Testing (MRI), Positron Emissions Tomography (PET) Scan and Magnetic Resonance Spectroscopy (MRS). A good resource for more information about diagnostic tests for epilepsy is the John Hopkins Hospital School of Medicine, Neurology and Neurosurgery,“Diagnosing Seizures and Epilepsy.”
Orthodox Treatments for Idiopathic Generalized Epilepsy
No cure for Idiopathic Generalized Epilepsy (IGE) currently exists so finding the proper treatment is very important to maintain a healthy lifestyle. People with IGE can live a normal life span.
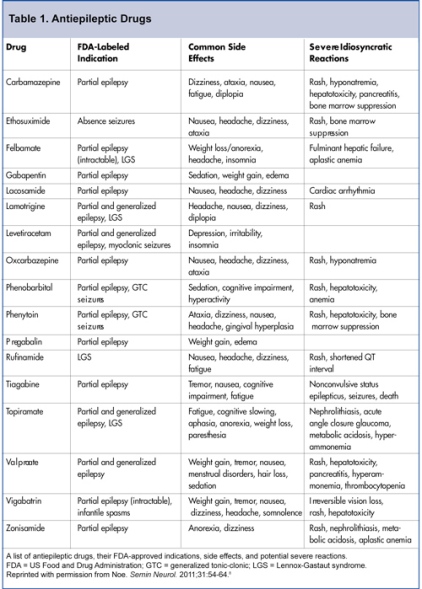
Prescription Drugs – Most patients diagnosed with idiopathic generalized epilepsy take medication to control their seizures. All prescription drugs have side effects. Some have potentially severe side effects. The medications to help control the incidence of seizures in patients with IGE include but are not limited to the following:
- Valproate
- Lamotrigine
- Topiramate
- Levetiracetam
- Ethosuximide
- Zonisamide
Alternative Treatments for Idiopathic Generalized Epilepsy
Alternative treatments for epilepsy include:
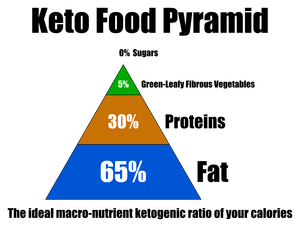
- Ketogenic Diet – A ketogenic diet may be considered to control IGE seizures. The diet is high in fat and low in carbohydrates. Ketones are formed when fat is used for the body’s source of energy. High ketone levels have been indicated to increase seizure control.
 Vining concludes, in a research review entitled “Tonic and atonic seizures: medical therapy and ketogenic diet. ” Epilepsia. 2009, that “Although these seizures are often very difficult to control, some of our medications/therapies have been shown to be effective. Recommendations concerning the efficacy of these therapies and a review of the newer therapies are provided. In addition, the ketogenic diet has been particularly successful in treating these seizures; this is discussed in some detail.”
Vining concludes, in a research review entitled “Tonic and atonic seizures: medical therapy and ketogenic diet. ” Epilepsia. 2009, that “Although these seizures are often very difficult to control, some of our medications/therapies have been shown to be effective. Recommendations concerning the efficacy of these therapies and a review of the newer therapies are provided. In addition, the ketogenic diet has been particularly successful in treating these seizures; this is discussed in some detail.”
Ketogenic diets have been successful with pediatric epilepsy in young children. Almost half of children and young people with epilepsy who have tried some form of this diet reduced seizures by at least 50% and maintained this decrease even after discontinuing the diet. Constipation, was the most common negative effect, affecting about 30% of patients, due to fluid restriction. This led to increased risk of kidney stones.
- Biofeedback– Biofeedback has been found to be an effective treatment for epilepsy. Relaxation techniques are used to control the body’s functions such as heart beat and blood pressure. Biofeedback may help control seizures that are triggered by stressful life events. In 10 research studies by Tan et al., (2009), Meta-analysis of EEG biofeedback in treating epilepsy, studied 87 patients whose seizures were not controlled by drug therapy.
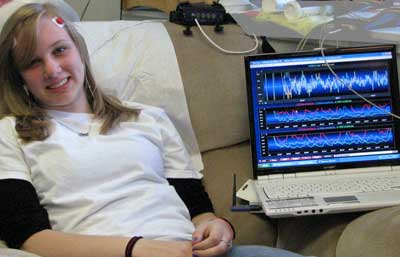 Those with contingent EEG biofeedback all the studies showed fewer weekly seizures and a significant reduction (P < 0.05) in the frequency of seizures. The researchers concluded that neurofeedback training is a possible treatment in patient whose seizures do not respond to medical therapies.
Those with contingent EEG biofeedback all the studies showed fewer weekly seizures and a significant reduction (P < 0.05) in the frequency of seizures. The researchers concluded that neurofeedback training is a possible treatment in patient whose seizures do not respond to medical therapies.
- Herbal remedies – Since ancient times, herbal remedies have been utilized in Traditional Chinese medicine for epilepsy.

In the US, herbal medicines are regulated by the 1994 Dietary Supplement and Health Education Act. Herbal remedies might be helpful in reducing the incidence of seizures, however, a study by Saper et al., 2004, “Heavy metal content of Ayurvedic herbal medicine products.” conducted in Boston with 70 herbal medicines found that 20% of these products contain potentially harmful levels of neurotoxic materials such as lead, mercury or arsenic that may cause seizures. 80% of the preparations did not contain harmful products, however. Some of the herbs that have been known to be effective in treating epileptic seizure side effects (nausea, headache, fatigue, etc.) are listed below:
Ailanthus altissima (Tree of Heaven)
Artemisia vulgaris (mugwort)
Calotropis procera (calotropis)
Cannabis sativa (marijuana)
Centella asiatica (hydrocotyle)
Convallaria majalis (lily of the valley)
Dictamnus albus (burning bush)
Paeonia officinalis (peony)
Scutellaria lateriflora (scullcap)
Senecio vulgaris (groundsel)
Taxus baccata (yew)
Valeriana officinalis (valerian)
Viscum album (mistletoe)
Gingko biloba, ephedra, eucalyptus, pennyroyal, shankhapusphi, star fruit, star anise & sage are some of the herbal medicines containing neurotoxic components which can induce seizures (Samuels et al., 2008), and should not be used by epileptic patients. More research is needed regarding the effectiveness of herbal remedies.
- Essential Oils – Essential oils can be effecting in calming the epileptic patient and preventing the symptoms of epilepsy. Such calming oils include: jasmine, ylang ylang, chamomile, and lavender (not spike lavender which is not recommended). Research was carried out at the University of Birmingham’s seizure clinic which involved using essential oils with individuals who had epilepsy.
 The studies used aromatherapy massage to allow individuals to associate the smell of an essential oil with a state of relaxation. Researchers concluded that the aroma triggers relaxation and can help to reduce seizures. According to the University of Maryland Medical Center, the following essential oils should be avoided: Eucalyptus (Eucalyptus globulus), Fennel (Foeniculum vulgare), Hyssop (Hyssopus officinalis), Pennyroyal (Mentha pulegium), Rosemary (Rosmarinus officinalis), Sage (Salvia officinalis), Tansy (Tanacetum vulgare), Thuja (Thuya occidentalis), and Wormwood (Artemesia absinthium) For more information about aromatherapy contact the Aromatherapy Council
The studies used aromatherapy massage to allow individuals to associate the smell of an essential oil with a state of relaxation. Researchers concluded that the aroma triggers relaxation and can help to reduce seizures. According to the University of Maryland Medical Center, the following essential oils should be avoided: Eucalyptus (Eucalyptus globulus), Fennel (Foeniculum vulgare), Hyssop (Hyssopus officinalis), Pennyroyal (Mentha pulegium), Rosemary (Rosmarinus officinalis), Sage (Salvia officinalis), Tansy (Tanacetum vulgare), Thuja (Thuya occidentalis), and Wormwood (Artemesia absinthium) For more information about aromatherapy contact the Aromatherapy Council
- Acupuncture -The effectiveness of acupuncture in treating epilepsy has not been statistically significant. A review of acupuncture in epilepsy, “Acupuncture for epilepsy” by Cheuk et al., (2009) included eleven randomized controlled trials. The authors suggested that studies using a larger sample size with appropriate standardized control groups are necessary to assess the effectiveness of acupuncture on treating epilepsy. They concluded that more studies are needed.
- Yoga– Yoga has been shown to be an effective treatment for epilepsy patients. In a research study conducted by Sathyaprabha et al., 2008, “Modulation of cardiac autonomic balance with adjuvant yoga therapy in patients with refractory epilepsy,” 18 members performed yoga (breathing exercise, meditation & yoga postures) and 16 members performed non-yoga exercise (quiet sitting & simple physical exercise) for one hour daily for 10 weeks.
 The researchers determined that the yoga group showed significant reduction in seizures (P<0.05) with improved parasympathetic parameters compared to no changes in the non-yoga exercise group. Thus it was concluded that yoga might be used effectively as an alternative therapy in management of autonomic dysfunction in patients with refractory epilepsy.
The researchers determined that the yoga group showed significant reduction in seizures (P<0.05) with improved parasympathetic parameters compared to no changes in the non-yoga exercise group. Thus it was concluded that yoga might be used effectively as an alternative therapy in management of autonomic dysfunction in patients with refractory epilepsy.
- Homeopathic Remedies – A few studies examined the effects of homeopathic remedies but were inconclusive. More research is needed. The following homeopathic remedies may be effective with eliminating associated epileptic symptoms (such as nausea, dizziness, and fever) and have no harmful side effects.
Belladonna — for seizures with a high fever
Causticum — for individuals with seizures triggered by feelings of sadness, grief, hopelessness and fear
Cicuta — for individuals with seizures after a head injury
Cuprum metallicum — for individuals with mental dullness; may be triggered by menstruation or vomiting
- Vitamin Supplements– Eating a well-balanced diet rich in vitamins and minerals may help maintain adequate mental function. People with epilepsy taking seizure medications do appear to have an increased need for calcium and vitamin D to help keep their bones healthy. Large doses of vitamin supplements, unsupervised, do not improve epilepsy and may even be harmful. Some epileptic medications can result in depletion of nutrients and vitamins. Folic acid supplements can be helpful in replenishing vitamin loss caused by medication.
 According to A.R. Gaby (2007), in a review entitled, “Natural Approaches to Epilepsy,” clinical observations and laboratory findings support the benefits of Vitamin E, magnesium, Manganese, thiamine (to improve cognitive function), folic acid, biotin, vitamin D, and L-Carnitine (to prevent valproate toxicitiy with epilepsy patients.
According to A.R. Gaby (2007), in a review entitled, “Natural Approaches to Epilepsy,” clinical observations and laboratory findings support the benefits of Vitamin E, magnesium, Manganese, thiamine (to improve cognitive function), folic acid, biotin, vitamin D, and L-Carnitine (to prevent valproate toxicitiy with epilepsy patients.
Vitamin E was found to be effective in reducing seizures in children according to a 1989 study conducted by Ogunmekan AO, MD. Twenty-four children age 6-17 were randomly assigned to 400 IU/day vitamin E or placebo for three months. of the 12 patients given vitamin E, 10 had a greater than 60% reduction in seizures. None of the placebo group had greater than 60% reduction. 6 out of the 12 children in the vitamin E group had 90-100% reduction in seizures. The study was statistically significant (p<0.05). People who not take take blood thinners should not take Vitamin E.
Other supplements such as Vitamin B6, taurine, vitamin K, melatonin and progesterone, were either uncontrolled trials or case reports, and may be effective with epilepsy symptoms, but more controlled studies and double blind studies are needed. There has been some research on the effects of omega-3 fatty acids on the reduction of epileptic seizures. Fish oil is mainly composed of omega-3 fatty acids (FAs), eicosapentaonoic acid (EPA) and docosahexaenoic acid (DHA). Pischon et al. (2003) concluded that increasing the intake of omega-3 FAs can reduce the plasma inflammatory markers and Schlanger (2002) concluded in a study entitled, “Diet enriched with omega-3 fatty acids alleviates convulsion symptoms in epilepsy patients,” that EPA could reduce seizures by decreasing these markers.
Always consult with your trusted health practitioner when making decisions regarding treatment. Alternative and complementary holistic health practices can be used in conjunction with orthodox or western medicine. Trust your own body wisdom and seek out professional advice.
Resources:
Center of Disease Control & Prevention
Epilepsy Foundation
Johns Hopkins Medicine
Epilepsy Society – Complimentary Therapies
NYU Langone Medical Center Comprehensive Epilepsy Center – Alternative Therapies
Epilepsy Health Center – Alternative Treatments to Epilepsy – WebMD
University of Maryland Medical Center -Seizure Disorders
National Center of Complementary and Alternative Medicine
Research References:
Benbadis S, and Heriaud L, “Idiopathic (Primary) Generalized Epilepsy,” Tampa General Hospital
Cheuk DKL, Wong V. Acupuncture for epilepsy (Review). Cochrane Database Syst Rev 2009; (4):CD005062.
Gaby AR, “Natural Approaches to Epilepsy,” (Review). Alternative Medicine Rev 2007; 12:1
Kossoff EH, Rho JM. Ketogenic diets: evidence for short- and long-term efficacy. Neurotherapeutics. 2009 Apr;6(2):406-14. Review.
Levy RG, Cooper PN, Giri P. Ketogenic diet and other dietary treatments for epilepsy. Cochrane Database Syst Rev. 2012 Mar 14;3:CD001903.
Li Q, Chen X, He L, Zhou D. Traditional Chinese medicine for epilepsy. Cochrane Database Syst Rev. 2009 Jul 8;(3):CD006454. Review.
Ogunmekan AO, Hwang PA. A randomized, double-blind, placebo-controlled, cllinical trial of d-alpha-trocopheryl acetate (vitamin E), as add-on therapy, for epilepsy in children. Epilepsia 1989;30:84-89.
Patel Y, and Welborn M, Alternative Therapies in Treating Epilepsy, ICE Epilepsy Alliance, Intractible Childhood Epilepsy
Pischon T, Hankinson SE, et al.: Habitual dietary intake of n-3 and n-6 fatty acids in relation to inflammatory markers among US men and women. Circulation 2003; 108:155–60.
Samuels N, Finkelstein Y, et al.: Herbal medicine and epilepsy: Proconvulsive effects and interactions with antiepileptic drugs. Epilepsia 2008, 49(3):373–380.
Saper RB, Kales SN, et al.: Heavy metal content of Ayurvedic herbal medicine products. JAMA 2004, 292:2868–2873.
Sathyaprabha TN, Satishchandra P, et al.: Modulation of cardiac autonomic balance with adjuvant yoga therapy in patients with refractory epilepsy. Epilepsy Behav 2008, 12:245-252.
Schlanger S, Shinitzky M, Yam D. Diet enriched with omega-3 fatty acids alleviates convulsion symptoms in epilepsy patients. Epilepsia 2002; 43:103–4.
Tan G, Thornby J, et al.: Meta-analysis of EEG biofeedback in treating epilepsy. Clinical EEG and neuroscience 2009, Vol.40 No. 3.
Vining EP. Tonic and atonic seizures: medical therapy and ketogenic diet. Epilepsia. 2009 Sep;50 Suppl 8:21-4. Review.
______________________________
 This article is written by Hang Pham and Jean Voice Dart. Hang Pham is a Monterey Bay Holistic Alliance Health and Wellness Educator. Hang Pham was born in Hoc Mon, Vietnam. She came to America in 1994, becoming a U.S. citizen in 2011. Hang graduated from Seaside High School with diploma and received her AA in General Studies from Monterey Peninsula College in 2011. She received her BA in Collaborative Health and Human Services from California State University Monterey Bay (CSUMB) in 2012. In addition to working as a volunteer staff with the Monterey Bay Holistic Alliance, she currently works as a Clerical Aid in the Human Resources Department of Salinas City Hall.
This article is written by Hang Pham and Jean Voice Dart. Hang Pham is a Monterey Bay Holistic Alliance Health and Wellness Educator. Hang Pham was born in Hoc Mon, Vietnam. She came to America in 1994, becoming a U.S. citizen in 2011. Hang graduated from Seaside High School with diploma and received her AA in General Studies from Monterey Peninsula College in 2011. She received her BA in Collaborative Health and Human Services from California State University Monterey Bay (CSUMB) in 2012. In addition to working as a volunteer staff with the Monterey Bay Holistic Alliance, she currently works as a Clerical Aid in the Human Resources Department of Salinas City Hall.
 Jean Dart, M.S. Special Education from Illinois State University, is a published author and has written hundreds of health articles as well as hosting a local television program, “Making Miracles Happen.” She is a Registered Music Therapist, Sound Therapist, and Master Level Energetic Teacher, and is the Executive Director, founder and Health and Wellness Educator of the Monterey Bay Holistic Alliance. To find out more about our Health Educators, or to apply as a Monterey Bay Holistic Alliance writer or volunteer, visit our website at www.montereybayholistic.com
Jean Dart, M.S. Special Education from Illinois State University, is a published author and has written hundreds of health articles as well as hosting a local television program, “Making Miracles Happen.” She is a Registered Music Therapist, Sound Therapist, and Master Level Energetic Teacher, and is the Executive Director, founder and Health and Wellness Educator of the Monterey Bay Holistic Alliance. To find out more about our Health Educators, or to apply as a Monterey Bay Holistic Alliance writer or volunteer, visit our website at www.montereybayholistic.com
Disclaimer: The Monterey Bay Holistic Alliance is a charitable, independent registered nonprofit 501(c)3 organization and does not endorse any particular products or practices. We exist as an educational organization dedicated to providing free access to health education resources, products and services. Claims and statements herein are for informational purposes only and have not been evaluated by the Food and Drug Administration. The statements about organizations, practitioners, methods of treatment, and products listed on this website are not meant to diagnose, treat, cure, or prevent any disease. This information is intended for educational purposes only. The MBHA strongly recommends that you seek out your trusted medical doctor or practitioner for diagnosis and treatment of any existing health condition.